What Is Cervical Cancer?
Cervical cancer starts in the cells of the cervix, the lower part of the uterus that connects to the vagina. Most cervical cancers are caused by long-term infection with human papillomavirus (HPV), a common virus spread through sexual contact.
Global Statistics
- Incidence & Mortality: In 2022, an estimated 661,021 women worldwide were diagnosed with cervical cancer, and it caused 348,189 deaths globally, making it the fourth most common cancer in women. The vast majority of these cases and deaths occur in low- and middle-income countries (sub-Saharan Africa, Central America and South-East Asia), where rates of incidence and mortality are significantly higher than in high-income countries, due to limited access to HPV vaccination, screening, and treatment. The primary cause of cervical cancer is persistent human papillomavirus (HPV) infection, which is a sexually transmitted virus. Women living with HIV are 6 times more likely to develop cervical cancer compared to the general population, and an estimated 5% of all cervical cancer cases are attributable to HIV.
Who Is at Risk?
- HPV infection (especially types 16 and 18)
- Smoking
- Weakened immune system
- Multiple sexual partners
- Early sexual activity
- Long-term use of birth control pills
- Lack of regular Pap or HPV tests
- Low access to screening or healthcare
Common Symptoms
Cervical cancer often has no symptoms in early stages. As it progresses, symptoms may include:
- Unusual vaginal bleeding (after sex, between periods, or after menopause)
- Unusual vaginal discharge (watery, pink, or foul-smelling)
- Pelvic or lower back pain
- Pain during sex / vaginal discomfort
- Longer or heavier periods
- Swelling in the legs
- Weight loss, fatigue and loss of appetite
Always see a healthcare provider if you experience these symptoms.
How Is It Diagnosed?
- Pap smear: Detects abnormal cervical cells
- HPV test: Checks for high-risk HPV types
- Colposcopy: A closer examination of the cervix using a special magnifying tool
- Biopsy: Confirms if abnormal cells are cancerous
- Imaging (MRI/CT/PET): To see if the cancer has spread
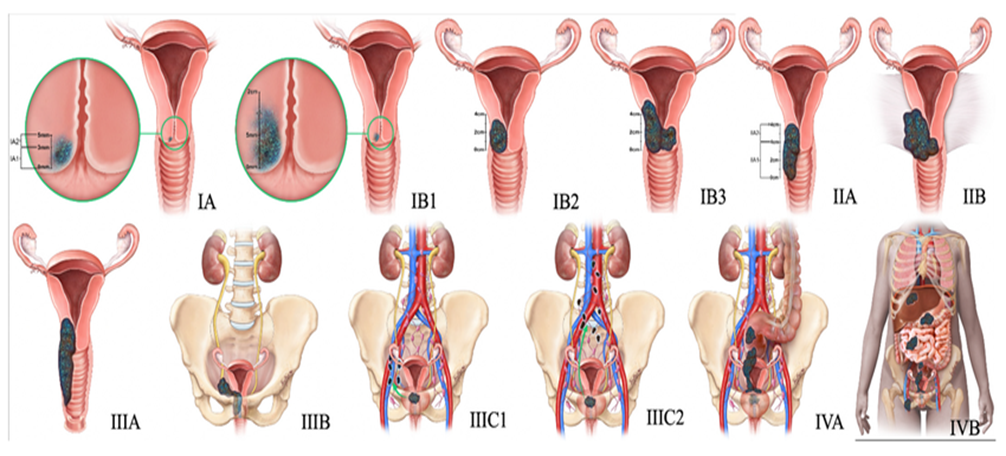
Staging of Cervical Cancer
- Stage I: Cancer is in the cervix only
- Stage II: Spread to nearby tissues
- Stage III: Spread to pelvic wall or lower vagina
- Stage IV: Spread to bladder, rectum, or distant organs
Staging helps guide treatment planning.
Treatment Options
Treatment depends on the stage, overall health, and if fertility preservation is desired:
Surgery
- For early-stage cancer (e.g., hysterectomy—removal of uterus and cervix)
- Fertility-preserving options may be available in very early stages
Radiation Therapy
- External or internal (brachytherapy) or combined depending on stage
- Often combined with concurrent chemotherapy for advanced stages
Chemotherapy
- Used with radiation or alone for advanced or recurrent cancer
Targeted Therapy
- Targets cancer growth factors (e.g., bevacizumab)
Immunotherapy
- Helps the immune system attack cancer cells
- Approved for advanced or recurrent cases with certain genetic features
Prevention and Screening
Boosting public awareness, access to information and services are key to prevention and control across the life course.
- HPV vaccination: Protects against cancer-causing HPV types (recommended for boys and girls from age 9–14)
- Routine Pap and HPV testing: Start by age 21 and repeat as advised
- Safe sexual practices: Limit partners, use protection
- Quit smoking
Early detection through regular screening saves lives.
WHO Response
All countries have made a commitment to eliminate cervical cancer as a public health problem. The WHO Global strategy defines elimination as reducing the number of new cases annually to 4 or fewer per 100 000 women and sets three targets to be achieved by the year 2030 to put all countries on the pathway to elimination in the coming decades:
- 90% of girls vaccinated with the HPV vaccine by age 15
- 70% of women screened with a high-quality test by ages 35 and 45
- 90% of women with cervical disease receiving treatment.
Modelling estimates that a cumulative 74 million new cases of cervical cancer can be averted, and 62 million deaths can be avoided by 2120 by reaching this elimination goal. Explore the cervical cancer knowledge repository for resources from WHO, UN agencies and other partners: Cervical cancer elimination initiative.
Living With Cervical Cancer
- Emotional and physical side effects can include fatigue, infertility, menopausal symptoms, and changes in sexual health
- Support services like counselling, physical therapy, and survivorship programs are available
- Regular follow-ups are important to monitor for recurrence or side effects
FAQs about Cervical Cancer
How is cervical cancer usually found?
Cervical cancer is diagnosed using a colposcopy to closely examine the cervix, often followed by a biopsy to take cell samples for laboratory analysis. A Pap test, which collects cells from the cervix, can detect abnormal cells. Other tests like imaging scans (CT, MRI, or PET-CT) are used to determine the extent of the cancer and its stage.
What is a Pap Test?
Pap Test (Cervical Screening): This is often the first step, where cells are collected from the cervix and examined for abnormalities.
What is the greatest risk for cervical cancer?
Human papillomavirus (HPV) infection is the most important risk factor for cervical cancer.
What is the most common age for cervical cancer?
Cervical cancer is most common in the age group of 30 to 34 years old in the UK, though it is most frequently diagnosed in women aged 35 to 44 in the US. Incidence rates rise sharply after age 15–19, peaking around this time before generally declining, though rates are increasing in younger adults in some areas.
Is cervical cancer hereditary?
No, cervical cancer is not considered a hereditary or directly inherited cancer, as it is primarily caused by persistent human papillomavirus (HPV) infection. While a family history of cervical cancer may be a risk factor, it's more likely due to shared environmental or lifestyle risk factors rather than a specific inherited gene. However, very rare genetic factors, such as a damaged DICER1 gene or inherited factors influencing immune response, might indirectly increase the risk of developing certain types of cervical cancer by affecting susceptibility to HPV.
How did my cervical cancer start?
Nearly all cervical cancers are caused by an infection with certain high-risk types of human papillomavirus (HPV). You can get HPV from: any skin-to-skin contact of the genital area. vaginal, anal or oral sex.
Where does cervical cancer first spread?
Cervical cancer most commonly spreads first to nearby lymph nodes in the pelvis before spreading further to distant organs like the lungs, liver, or bones. Cancer can also spread to nearby pelvic organs such as the bladder or rectum.
Is cervical cancer painful?
Yes, cervical cancer can cause pain in the lower back, between the hip bones (pelvic area), or in the lower tummy (abdomen), and also pain during or after sex, especially as it progresses. However, early-stage cervical cancer often has no symptoms, and pain can also be a sign of other, less serious conditions, so it's crucial to see a doctor for any persistent or unexplained pain.
Can cervical cancer be cured?
Yes, cervical cancer can be cured, particularly if caught and treated in its early stages through treatments like surgery, radiation, or chemotherapy. Early detection is crucial for a successful outcome and improved quality of life, which is why screening and HPV vaccination are so important. For more advanced cases, the goals of treatment shift to controlling the disease and managing symptoms, though in some cases, a cure is still possible.
Where can I find a Specialist for Cervical Cancer?
You can search your Cervical Cancer Specialist / Gynae-Oncologist on www.ioncosolutions.com