What Is Pancreatic Cancer?
Pancreatic cancer starts in the pancreas , an organ located behind the stomach that helps with digestion and blood sugar regulation. The majority of pancreatic cancers begin in the exocrine cells , which produce digestive enzymes, and are called adenocarcinomas .
There are two main types:
- Exocrine tumours (Adenocarcinomas): The most common type (around 95% of cases).
- Endocrine tumours (Pancreatic Neuroendocrine Tumours or PNETs): A rarer form that starts in the hormone-producing cells of the pancreas.
Global Bowel Cancer Statistics
- Incidence: Pancreatic cancer is the 10th most common cancer globally , with an estimated 308,000 new cases diagnosed in 2020.
- Mortality: Approximately 241,000 deaths occur annually due to pancreatic cancer, making it the seventh leading cause of cancer-related death worldwide.
- Survival Rates: The five-year survival rate for pancreatic cancer remains around 13% , highlighting the challenges in early detection and effective treatment.
Who Is at Risk?
The following factors may increase your risk of developing pancreatic cancer:
- Age: Risk increases after age 60
- Smoking: Smokers are 2 to 3 times more likely to develop pancreatic cancer.
- Obesity and high-fat diet
- Family history : Genetic mutations, such as BRCA2 , or a family history of pancreatic cancer increases the risk.
- Chronic pancreatitis: Long-term inflammation of the pancreas
- Diabetes: Type 2 diabetes is associated with a higher risk of developing pancreatic cancer
- Genetic syndromes: Such as Lynch syndrome, Peutz-Jeghers syndrome , and familial atypical multiple mole melanoma (FAMMM)
Common Symptoms
Pancreatic cancer is often diagnosed at later stages because early symptoms can be vague. Symptoms may include:
- Jaundice (yellowing of the skin or eyes).
- Abdominal pain or discomfort, often radiating to the back.
- Unexplained weight loss
- Losing of appetite
- Fatigue
- Nausea and vomiting
- New-onset diabetes or worsening of existing diabetes
- Changes in stool (light-colored, greasy, or floating)
If you experience persistent symptoms, it's important to seek medical attention.
How Is Pancreatic Cancer Diagnosed?
- Blood tests: Elevated levels of CA 19-9, a tumour marker, can indicate pancreatic cancer (though not always accurate).
- Imaging tests:
- CT scan or MRI: To visualize the tumour and check for metastasis
- Endoscopic ultrasound (EUS): To obtain tissue samples for biopsy
- Endoscopic retrograde cholangiopancreatography (ERCP): A procedure to check the bile ducts and pancreas
- Biopsy: A tissue sample may be taken to confirm cancer.
- Laparoscopy A surgical procedure to view the pancreas directly, sometimes used to stage cancer
Stages of Pancreatic Cancer
Stage I: Cancer is confined to the pancreas.
Stage II: Cancer has spread to nearby lymph nodes or tissues
Stage III: Cancer has spread to major blood vessels and nearby organs
Stage IV: Cancer has spread to distant organs, such as the liver, lungs, or peritoneum
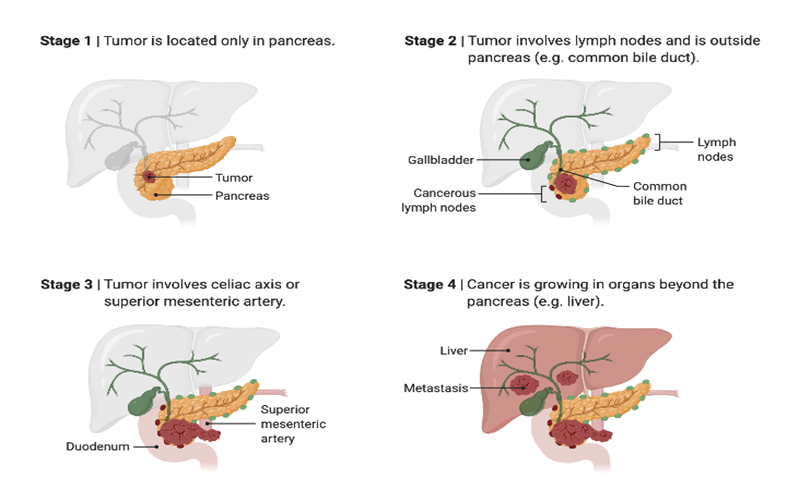
Staging helps determine the best course of treatment.
Treatment Options
Treatment depends on the cancer stage, location, and overall health of the patient. Common treatment options include:
Surgery
- Whipple procedure (pancreaticoduodenectomy): The most common surgery for pancreatic cancer, where part of the pancreas, bile duct, and nearby organs are removed.
- Distal pancreatectomy: Removal of the body and tail of the pancreas.
- Total pancreatectomy : Removal of the entire pancreas (less common).
Surgery is typically only an option for tumours confined to the pancreas and can improve survival chances.
Chemotherapy
- Chemotherapy drugs are used to shrink tumours, kill cancer cells, and prevent cancer from spreading. Common regimens include FOLFIRINOX and Gemcitabine (sometimes combined with other drugs).
- Chemotherapy can also be used before or after surgery to improve outcomes.
Radiation Therapy
- High-energy radiation is used to target and kill cancer cells.
It's often combined with chemotherapy or used for patients who can't undergo surgery.
Targeted Therapy
- Erlotinib (Tarceva): Approved for pancreatic cancer in combination with gemcitabine in advanced cases. Targeted therapies focus on specific molecular markers in cancer cells to stop their growth.
Immunotherapy
- Immunotherapy, like Keytruda (pembrolizumab) , is an emerging treatment, particularly for cancers with specific genetic mutations, such as microsatellite instability-high (MSI-H) tumours.
- This approach stimulates the body's immune system to attack cancer cells.
Palliative Care
- Focuses on symptom management and improving the quality of life for patients with advanced pancreatic cancer. Pain relief, nutritional support, and counselling are essential parts of care.
Living With Pancreatic Cancer
- Emotional and psychological support: It's important to have emotional support from family, friends, or support groups. Pancreatic cancer can be challenging emotionally, and counselling may be beneficial.
- Nutrition: Pancreatic cancer can affect digestion and nutrient absorption. Nutritional support and changes in diet may help manage symptoms and improve well-being.
- Pain management: Effective pain relief is crucial for comfort, especially in advanced stages.
Prevention
While there's no guaranteed way to prevent pancreatic cancer, lifestyle changes may reduce the risk:
- Quit smoking: Smoking is a major risk factor.
- Maintain a healthy weight: Reducing obesity risk through diet and exercise.
- Healthy diet: A diet rich in fruits, vegetables, and whole grains and low in red meat and processed foods may lower the risk.
- Regular medical check-ups: For those with genetic risk factors or a family history of pancreatic cancer, regular screenings may be recommended.
Advances in Diagnosis and Research
1. Early Detection Innovations
PAC-MANN Blood Test: Researchers at Oregon Health & Science University have developed an inexpensive blood test called PAC-MANN, which detects pancreatic cancer with 85% accuracy, even in its early stages. The test measures changes in protease enzyme activity and costs less than a penny per sample, making it accessible for underserved areas.
AI-Powered Imaging Tools: Northwell Health has introduced an AI-powered tool named iNav, which analyses MRI and CT scans to identify early signs of pancreatic cancer. This proactive approach has reduced the time from diagnosis to treatment by 50%.
2. Targeted Therapies
KRAS Inhibitors: Pancreatic cancer is characterized by mutations in the KRAS gene. New treatments targeting this mutation, such as daronrasib, have shown promise in early trials, offering extended survival for patients with advanced stages of the disease.
NRG1 Fusion Targeted Therapy: The FDA approved Merus NV's therapy, Bizengri (zenocutuzumab), for treating pancreatic cancers linked to the NRG1 gene fusion. This therapy blocks the interaction between the HER3 protein and the NRG1 gene, inhibiting tumour growth.
3. Adjunctive Treatments
High-Dose Vitamin C: A study by the University of Iowa Health Care Carver College of Medicine found that administering 75 grams of vitamin C thrice weekly significantly enhanced the efficacy of chemotherapy for pancreatic cancer patients, doubling overall survival from 8 months to 16 months. .
Treatment Innovations
1. Combination Chemotherapy
Irinotecan Liposome-Based Regimen: The FDA approved irinotecan liposome in combination with oxaliplatin, fluorouracil, and leucovorin as a first-line treatment for metastatic pancreatic adenocarcinoma. This regimen has shown improved efficacy compared to traditional treatments.
2. Minimally Invasive Procedures
Irreversible Electroporation (IRE): IRE is a non-thermal ablation technique used to treat locally advanced pancreatic cancer. Clinical data suggest that IRE, when combined with chemotherapy, can improve survival rates and reduce tumour size. However, it remains a high-risk procedure requiring additional safety data before widespread use.
FAQs about Bowel Cancer
What is the life expectancy of a person with pancreatic cancer?
Pancreatic cancer has a poor prognosis, with only about 8.3% of people in England diagnosed between 2016-2020 surviving for five years or more. Survival rates vary significantly by stage; for example, a localized (early-stage) tumour in the US has a 44% five-year survival rate, while a distant (late-stage) tumour has a 3% rate. A major reason for the low survival is the late diagnosis, as symptoms often don't appear until the cancer has grown significantly or spread.
What feeds pancreatic cancer?
Pancreatic cancer cells feed off hyaluronic acid. Often found in beauty products and wellness supplements, hyaluronic acid attracts and retains water well. It's also a major player in the physiology of pancreatic tumours.
How long can you have pancreatic cancer without knowing?
Pancreatic cancer can be present for years without being detected because it often has no early symptoms or causes vague symptoms that are mistaken for other conditions.
What is the main cause of pancreatic cancer?
While there is no single cause for pancreatic cancer, the main risk factors include smoking, chronic pancreatitis (long-term inflammation of the pancreas, often from alcohol), obesity, and a family history of the disease. Other factors that can increase risk are a diet high in processed meats and fats, developing diabetes, and long-term exposure to certain industrial chemicals.
How fast does pancreatic cancer go from stage 1 to stage 4?
Pancreatic cancer progression is highly variable, but some studies suggest it can take just over a year for an early-stage (Stage 1) tumor to progress to Stage 4, though the overall development from a pre-cancerous cell to a potentially fatal cancer can take decades.
What age do most people get pancreatic cancer?
Pancreatic cancer is most common in middle to older age, with most cases diagnosed in people over 65, and especially in those aged 75 and over.
Does alcohol cause pancreatic cancer?
Yes, alcohol is associated with an increased risk of pancreatic cancer, with the risk growing with higher consumption levels, particularly heavy drinking.
Where can I find a Specialist for Pancreatic Cancer?
You can search your Pancreatic Cancer Specialist on www.ioncosolutions.com