What Is Liver Cancer?
Liver cancer begins in the cells of the liver, an organ located in the upper right part of your abdomen that plays a vital role in digestion, metabolism, and detoxification.
There are two main types of liver cancer:
- Primary liver cancer: The cancer starts in the liver cells. The most common form is hepatocellular carcinoma (HCC) , which makes up about 75% of liver cancers.
- Secondary liver cancer (metastatic liver cancer): This Occurs when cancer from another part of the body (like the colon, breast, or lungs) spreads to the liver.
Global Statistics
- Incidence & Mortality: In 2020, there were an estimated 905,700 new cases and 830,200 deaths from liver cancer globally. It is the third leading cause of cancer-related death worldwide.
- Projected Increase: By 2040, new cases and deaths are expected to rise by over 55%, potentially reaching 1.4 million cases and 1.3 million deaths annually.
- Regional Disparities: Highest rates occur in Eastern Asia, Northern Africa, and South-Eastern Asia, with men being more affected than women.
Who Is at Risk?
Certain factors increase the risk of developing liver cancer, including:
- Chronic liver disease: Hepatitis B or C, cirrhosis, and fatty liver disease are major risk factors.
- Alcohol consumption: Excessive and long-term drinking can lead to liver damage, increasing the risk of liver cancer.
- Obesity and non-alcoholic fatty liver disease (NAFLD): These are linked to the development of cirrhosis and liver cancer.
- Type 2 diabetes: Increases the likelihood of liver disease, which can lead to cancer.
- Family history : Having a family member with liver cancer increases your risk.
- Exposure to aflatoxins: These are toxins produced by fungi found in improperly stored grains and nuts, and they can increase the risk of liver cancer.
Common Symptoms
Early-stage liver cancer often doesn’t cause symptoms. However, as the disease progresses, symptoms may include:
- Pain or discomfort in the upper right side of the abdomen
- Unexplained weight loss
- Loss of appetite
- Jaundice (yellowing of skin or eyes)
- Fatigue
- Nausea or vomiting
- Swollen abdomen (due to fluid accumulation)
- Dark urine or pale stools
If you experience any of these symptoms, it’s essential to seek medical attention, especially if you have risk factors.
How Is Liver Cancer Diagnosed?
Liver cancer is often diagnosed using a combination of the following tests:
Blood tests: Tests like alpha-fetoprotein (AFP) , a tumour marker, can help detect liver cancer. However, elevated AFP levels can also be caused by other liver diseases.
- Imaging tests:
- Ultrasound: A non-invasive way to look for tumours in the liver.
- CT scan or MRI: Provides detailed images of the liver and helps in staging the cancer.
- Elastography (FibroScan): Measures liver stiffness to determine the degree of liver damage or cirrhosis
- Biopsy: A small sample of liver tissue may be taken to confirm cancer.
- Laparoscopy: A surgical procedure that allows a doctor to view the liver directly and obtain tissue samples.
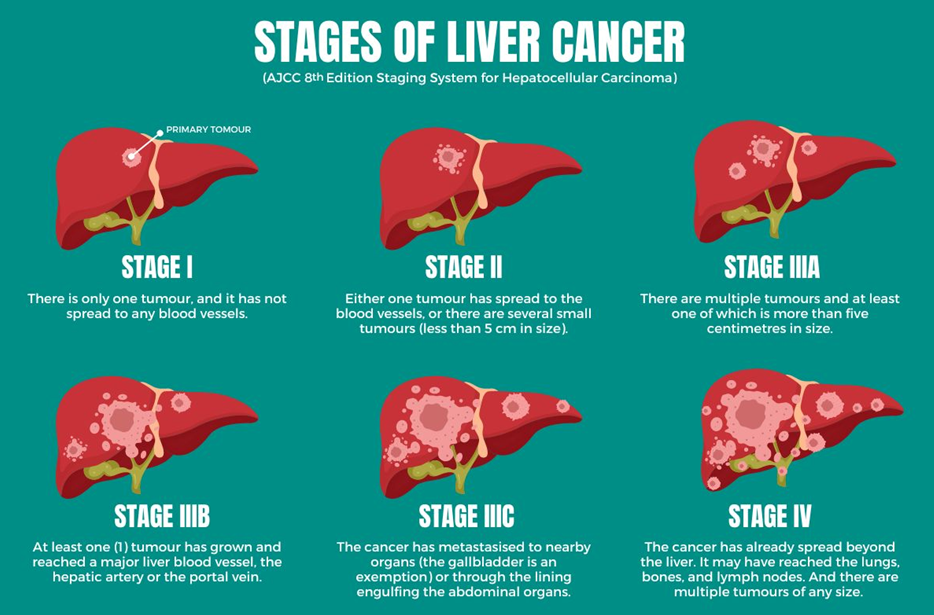
Stages of Liver Cancer
- Stage I: The tumour is confined to one part of the liver.
- Stage II: The cancer has grown, or multiple tumours are present but still confined to the liver.
- Stage III: The cancer has spread to nearby lymph nodes or blood vessels.
- Stage IV: The cancer has spread to distant organs, such as the lungs or bones.
Treatment Options
The choice of treatment depends on the size, location, and spread of the tumour, as well as the overall health of the patient.
Surgery
- Liver resection: : Removal of the part of the liver that contains the tumour. This is an option for patients with early-stage liver cancer and healthy liver tissue remaining.
- Liver transplant: In cases of advanced liver cancer or cirrhosis, a liver transplant may be necessary. The entire liver is replaced with a healthy liver from a donor.
Ablation Therapy
- Radiofrequency ablation (RFA):Uses heat to destroy cancer cells. It’s usually used for small tumours or when surgery isn’t possible.
- Percutaneous ethanol injection (PEI) : Alcohol is injected directly into the tumour to destroy cancer cells.
- Microwave ablation: Similar to RFA, this technique uses microwave energy to heat and destroy cancer cells.
Transarterial Chemoembolization (TACE)
- A procedure that delivers chemotherapy directly to the tumour by injecting it into the blood vessels that supply the liver. It also cuts off the tumour’s blood supply, causing it to shrink.
Radiation Therapy
- Uses high-energy rays to kill cancer cells. It’s typically used in advanced stages or when surgery is not an option.
Chemotherapy
- Systemic chemotherapy: Used in cases where cancer has spread. It’s generally not very effective for liver cancer, but newer drugs and combinations are being tested.
Targeted Therapy
- Sorafenib : The first FDA-approved targeted therapy for advanced liver cancer, it works by blocking the signals that allow cancer cells to grow.
- Lenvatinib : The first FDA-approved targeted therapy for advanced liver cancer, it works by blocking the signals that allow cancer cells to grow.
Immunotherapy
- Drugs like nivolumab and pembrolizumab are being used to treat advanced liver cancer. These drugs work by stimulating the immune system to attack cancer cells.
Clinical Trials
- New treatments for liver cancer are constantly being tested in clinical trials. Participating in a trial can give patients access to new therapies before they become widely available.
Living With Liver Cancer
- Fatigue: This is a common symptom of liver cancer and its treatments. Rest and energy management are crucial.
- Nutritional support: Patients may experience difficulty eating due to pain, nausea, or loss of appetite. Working with a nutritionist to maintain strength and avoid malnutrition is important.
- Psychosocial support: Liver cancer can be emotionally overwhelming. Counselling or support groups may help patients cope with anxiety, depression, or stress.
- Follow-up care: Regular check-ups are essential to monitor for recurrence and manage any ongoing side effects.
Prevention
While liver cancer can’t always be prevented, certain lifestyle changes and medical interventions can help reduce your risk:
- Vaccination: Getting vaccinated for hepatitis B can reduce the risk of liver cancer.
- Avoid excessive alcohol use: Limiting alcohol intake can reduce the risk of liver damage and cancer.
- Healthy diet and weight management: A balanced diet and regular exercise can help prevent fatty liver disease and liver cancer.
- Treating underlying liver conditions: Managing hepatitis B or C, cirrhosis, and fatty liver disease with medication and regular monitoring can lower the risk.
Advances in Diagnosis and Research
1. Early Detection Innovations
LiverFormer Model: A deep learning model called LiverFormer has been developed to enhance the precision of liver cancer treatment planning. It accurately segments liver sub-regions, aiding in targeted therapies and reducing damage to healthy tissue.
2. Molecular Subtyping
DLSOM Framework: Researchers introduced DLSOM , a deep learning framework that analyses somatic mutations to identify five distinct liver cancer subtypes. This approach could lead to more personalized treatment strategies based on genetic profiles in future.
Treatment Innovations
1. Combination Therapies
TACE + Immunotherapy: Combining Transarterial Chemoembolization (TACE) with immune checkpoint inhibitors like Durvalumab and Bevacizumab has shown promising results. In a recent trial, this combination nearly doubled the median progression-free survival time to 15 months, compared to 8 months with placebo.
2. Non-Invasive Treatment
Histotripsy: A non-invasive technique called histotripsy uses high-intensity sound waves to destroy liver tumours. It received FDA clearance in October 2023 and has been used on over 300 patients. An eight-year study is underway to assess its long-term efficacy.
3. New Drug Approvals
Cabozantinib: In Scotland, Cabozantinib has been approved for treating advanced hepatocellular carcinoma (HCC), offering a new option for patients who cannot undergo surgery.
FAQs about Liver Cancer
At what age do most people get liver cancer?
Although liver cancer can happen at any age, it is most common in older people. Most people diagnosed are over the age of 60. The highest rates are in 85 to 89 year olds.
What is the main cause of liver cancer?
Liver cancer is often caused by long-term liver damage from hepatitis B or C infection, excessive alcohol, or obesity-related fatty liver disease. Other risk factors include exposure to aflatoxins (a type of fungus) and certain chemicals, a family history of liver cancer, diabetes, and smoking. In some cases, the cause is unclear, but many cases develop from cirrhosis, a condition where the liver becomes damaged and scarred.
How to reduce liver cancer risk?
Many liver cancers could be prevented by reducing exposure to known risk factors for this disease.
- Preventing hepatitis B (HBV) and C (HCV) infections.
- Avoid or limit alcohol and tobacco use.
- Get to and stay at a healthy weight.
- Limit exposure to cancer-causing chemicals.
- Treat diseases that increase liver cancer risk.
Is liver cancer hereditary?
Liver cancer is not typically considered a highly hereditary cancer, though having a close family member with the disease can increase your risk. This increased risk may stem from shared genetic factors, shared environmental factors, or a combination of both. While acquired gene mutations in liver cells are a common cause of liver cancer, certain inherited conditions, such as hemochromatosis, can increase susceptibility to liver cancer.
Where does liver cancer usually start?
Liver cancer begins in the cells of the liver. The most common form of liver cancer begins in cells called hepatocytes. This type of cancer is called hepatocellular carcinoma.
How often should I get screened for liver cancer?
For people at higher risk of liver cancer because they have cirrhosis (from any cause), hereditary hemochromatosis, or chronic hepatitis B infection (even without cirrhosis), some experts recommend screening for liver cancer with alpha-fetoprotein (AFP) blood tests and ultrasound exams every 6 months.
What is the best treatment for liver cancer?
There isn't a single "best" treatment for liver cancer; the most effective approach depends on the stage of the cancer and the patient's overall health, especially the function of their liver. Early-stage cancers are often treated with surgery to remove the tumour or a liver transplant. For early to advanced tumours, tumour ablation (destroying cells with heat) is an option. Other treatments include chemoembolisation (cutting off blood supply with chemotherapy)or radioembolisation (using radiation), systemic drug treatments (chemotherapy / immunotherapy), or radiotherapy.
What is the best diet for liver cancer patients?
A liver cancer diet emphasizes nutrient-dense foods to support healing and function, including lean proteins, whole grains, fruits, and vegetables. Prioritize foods rich in antioxidants and fibre like berries, leafy greens, and whole grains. Protein sources such as fish, poultry, tofu, and beans are crucial for rebuilding tissues. Healthy fats from avocados, nuts, and seeds are also beneficial. Limit foods high in saturated fats, trans fats, and salt.
How long can you live with liver cancer?
Survival with liver cancer varies significantly, ranging from several years for early-stage cases that can be cured with surgery or transplant to much shorter periods for advanced stages, with median survival for stage C being 11-13 months and even less for stage D without treatment. Factors such as the stage of the cancer, its size, whether it has spread, the overall health of the liver, and the type and effectiveness of treatment all influence life expectancy.
Where can I find a Specialist for Liver Cancer?
You can search your Liver Cancer Specialist on www.ioncosolutions.com